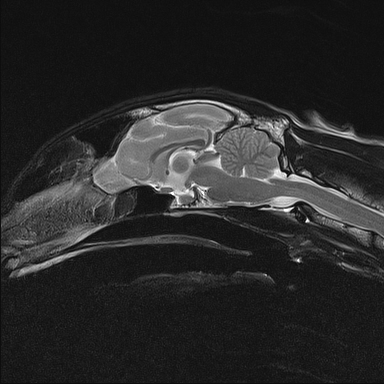
What is feline orofacial pain syndrome (FOPS)?
Feline orofacial pain syndrome is a disease characterised by face and tongue mutilation and other behavioural signs suggesting oral and facial discomfort (for example exaggerated licking and chewing movements). The apparent discomfort and/or mutilation are disproportionate to any possible causes for the pain (for example teething). The disease is most likely a neuropathic pain disorder similar to trigeminal neuralgia in humans.
What type of cat is affected by FOPS and what are the clinical signs?
FOPS is characterised by face and tongue discomfort and affected cats are most commonly presented with exaggerated licking and chewing movements with pawing at the mouth also. More severe cases may mutilate their tongue and lips and in the most severe cases may even require surgery to repair tongue tears. Typically, the discomfort seems to be worse on one side. The apparent discomfort is often episodic and bouts of pain can be triggered by tongue movement for example during grooming, eating or drinking. Bouts of pain can last between several minutes to several hours and are often preceded by a short period of behaviour suggesting anxiety. Some cats are in more continuous discomfort, are at greater risk of mutilation and may also be anorexic or unwilling to eat. FOPS is most common in the Burmese cat, however, the disease may be seen in any variety including Siamese, Tonkinese, Burmilla, and the domestic shorthair, it is thought FOPS is an inherited condition. Any age of cat can be affected however many affected cats will first show clinical signs when erupting permanent teeth i.e. teething. Oral lesions, especially dental disease, and environmental stress can precipitate the condition.
What is the cause of FOPS?
FOPS has similarities to trigeminal neuralgia in humans and is a neuropathic pain disorder i.e. pain due to abnormal nervous system processing of pain messages. The trigeminal nerve conveys sensory information, e.g. pain and touch around the face and mouth to the brain. It is suggested that affected cats have misfiring of this nerve. In FOPS when the nerve fires, for example during teething or dental disease, it sends an inappropriately large message of pain. Conditions of neuropathic pain can be greatly influenced by environmental factors (imagine if you have a headache – it can be made worse by stress). The most common environmental factor that can trigger FOPS is stressful interaction with other cats, for example, house mates or neighbourhood cats invading the home and garden territory. Visits, for example to shows, veterinary practices and catteries, can also be a trigger.
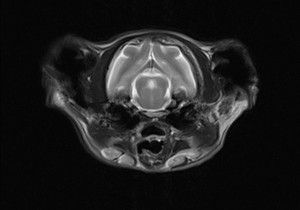
How is FOPS diagnosed?
There is no definite diagnostic test for this disease and the diagnosis is made on the basis of the characteristic clinical signs, elimination of other explanations and identification of contributing causes.
1. Ruling out other causes of facial and oral pain
- Medical examination: Your primary care vet will examine your cat for other causes of mouth pain in particular dental disease. Dental disease will cause the cat to be distressed. However, the difference between FOPS and more straightforward dental disease is that in FOPS the response to the pain is inappropriate and characterised by mutilation. Your veterinarian may recommend other tests such as blood work or radiographs.
- Neurological examination: Although FOPS is thought to be due to misfiring of the trigeminal nerve, tests to examine the function of this nerve will be normal. These tests include lightly touching your cat’s face, eyes and lips to ascertain whether feeling is present. The presence of neurological problems such as a failure to feel touch or close the mouth is not consistent with FOPS. Your primary care vet may at this point recommend referral to Fitzpatrick Referrals to have an appointment with one of our neurology clinicians for further assessment. Tests to investigate the trigeminal nerve specifically may be recommended e.g. magnetic resonance imaging (MRI).
2. Investigation and treating dental disease
- The majority of cases of FOPS are triggered by periodontal disease and it is essential that this is investigated and treated even if on causal inspection the cat only seems to have a little gingivitis (inflammation of the gums). Remember in FOPS the trigeminal nerve sends out an inappropriate message and so even apparently minor dental disease should be treated. Cats are predisposed to feline oral resorptive lesions (FORLs) which may be hidden under plaque or the swollen gum. FORLs are characterised by loss of the tooth enamel and exposure of the sensitive pulp and are very painful. It is very important to identify and treat dental disease promptly. Your primary care vet is most likely to recommend radiographs of the teeth and may suggest referral to a veterinary dental specialist.
3. Identifying environmental stress and triggers
- As environmental factors can influence FOPS it is important to look for possible contributory factors for example social stress. Identification of social incompatibility in a multi-cat household is a key step.
Factors to consider include:
- Does the cat have its own secure core territory (i.e. own litter tray, feeding area and private space)?
- Visual access into the home, for example, can the affected cat see another cat through a window?
- Points of entry and exit, for example, does another cat block access going in, out or even within a territory?
- Is there adequate provision of privacy?
- Is the cat able to use its natural behavioural strategies for coping with stress – such as hiding, elevation and distancing?
How is FOPS treated?
The main aim of treating FOPS is to reduce the discomfort, limit the mutilation and identify and treat or prevent the underlying triggers.
- Preventing mutilation: Until discomfort can be controlled, mutilation should be prevented by using an Elizabethan collar and / or paw bandaging. This is a painful disorder and merely preventing your cat from mutilation without attempting to prevent the discomfort is inappropriate.
- Identify and treat dental disease
- Identify and reduce environmental stress: It is essential that there is appropriate distribution of the five essential feline resources – food, water, resting places, litter tray and points of entry and exit into the territory. Your cat should also have a private area(s) and the ability to hide and elevate themselves in order to control stress. Use of commercially available diffusers or sprays containing feline facial pheromone F3 or Valerian essential oil can be useful.
- Reduce discomfort: Your cat may be prescribed drugs to reduce discomfort. For mild cases, these may include non-steroidal anti-inflammatory drugs such as meloxicam and / or opioids such as buprenorphine. However, these common painkillers are not always effective for neuropathic pain and consequently, your primary care vet or neurology clinician may recommend unlicensed drugs. Drugs used to treat neuropathic pain are typically anti-epileptic drugs such as phenobarbital, carbamazepine, gabapentin or antidepressants such as amitriptyline. These drugs reduce misfiring of nerves and consequently reduce pain.
What is the prognosis of FOPS?
Classically FOPS is an episodic condition, at least initially. The first episode may be seen at teething and the second may not be until your cat develops periodontal disease later in life. After starting treatment, the discomfort should lessen within 3 days and is usually absent or infrequent after 7 days of therapy. Attempts should be made to wean off medication after 4 weeks especially if the predisposing causes have been treated or have resolved. For immature cats erupting permanent teeth, the discomfort will resolve when the permanent dentition is fully erupted. Seek veterinary advice before withdrawing any medication – sudden discontinuation of phenobarbital can cause withdrawal seizures.
Unfortunately in a proportion of cats, the signs of FOPS become continuous i.e. there is no remission and long-term therapy is required. In addition, pain can be more difficult to treat and sometimes more than one drug is necessary to control the discomfort. Kittens which present with FOPS during teeth eruption are highly likely to re-present as older cats, therefore, prophylactic dental health care, maintaining oral health and preventing periodontal disease is advised. Environmental stress should also be limited. The number of cats within the household should be restricted to socially compatible levels and careful attention should be paid if further cats are to be introduced.
Can I breed my cat or its relatives?
FOPS is thought to be inherited and an autosomal recessive inheritance would fit with the limited data that is available. An autosomal recessive inheritance would mean that both Tom and Queen of an affected cat either have or carry the condition. Because environmental factors such as dental disease and stress influence the disease not every cat with an affected genotype will necessarily have clinical signs. In addition, the signs of the disease might occur after the cat has been bred. This makes it particularly difficult for a pedigree cat breeder to select disease-free stock and it is hoped that ultimately the disease gene can be identified to enable easy screening. In the meantime, breeders are advised not to breed any cat which has had signs of the disease even if the signs are not persistent. Breeding the Tom and Queen of affected cats is also not advised, especially the Tom as his genetic influence can be so far-reaching.
7 minute read
In this article