Whilst osteosarcoma is the most common bone tumour affecting dogs and cats, other, generally less aggressive / less malignant tumours can also occur, such as chondrosarcoma and fibrosarcoma, for which the survival time is generally longer.
Osteosarcoma
What is canine osteosarcoma (OSA)?
OSA is a malignant tumour of bone and it is the most common bone tumour found in dogs. It mostly affects the limbs (appendicular skeleton), but it can also develop in the skull, spine and ribs (axial skeleton).
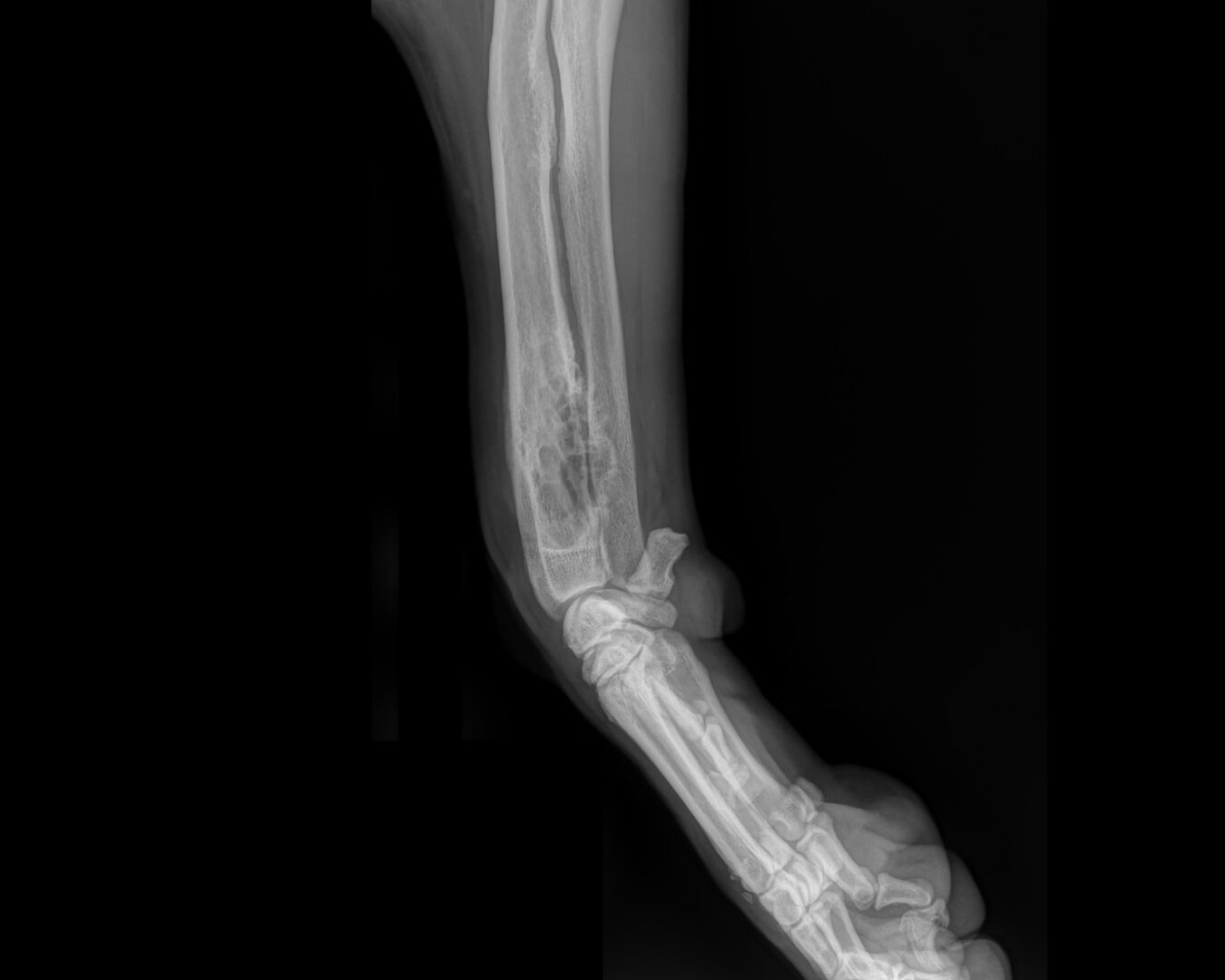
The tumour often occurs in the front legs, where it most commonly affects the bottom part of the radius (just above the wrist joint) and less commonly, the top of the humerus. OSA can also occur in the femur and tibia of the hind limb.
OSA can occur at any age and in any breed but it usually develops in older, large and giant breeds.
How can I tell if my dog has an OSA?
Appendicular
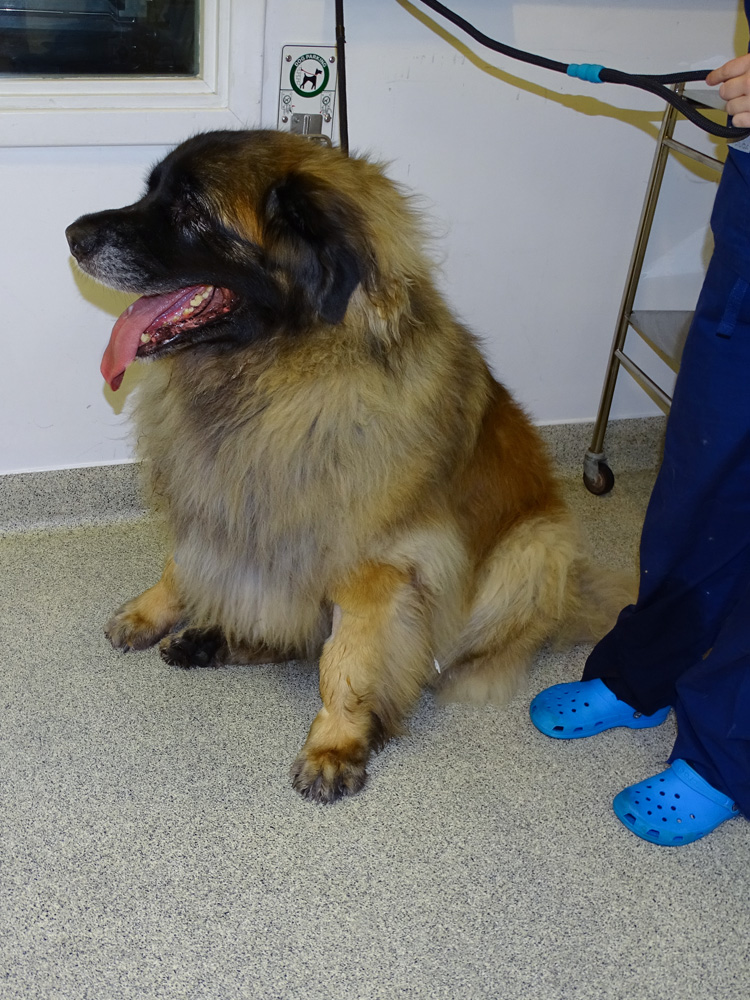
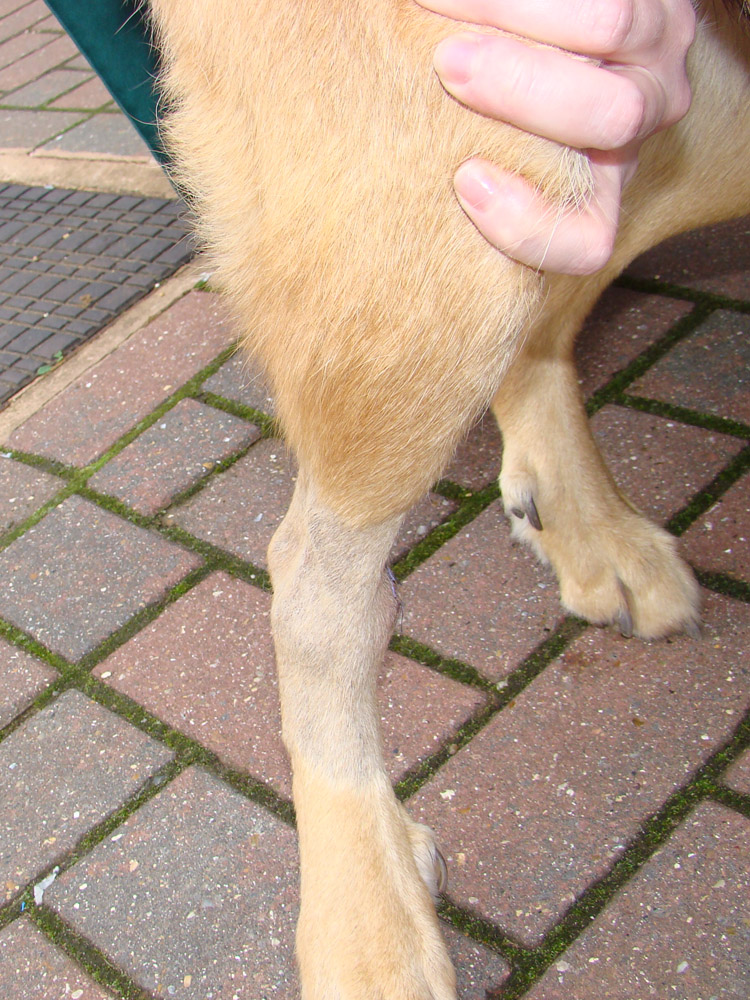
If OSA is affecting your dog’s leg you may or may not have noticed a local firm swelling in the limb. You may also, or only, have noticed that your dog has developed a lameness which is persistent and does not resolve with rest, or even with painkillers.
OSA is a painful condition since the tumour is expanding within the bone, so dogs may also be showing signs of restlessness. However, some dogs are extremely brave and hide pain remarkably well, so they may only be exhibiting subtle behavioural changes, which only you may be able to identify, e.g. loss of appetite, shaking or shivering, change in demeanour and reduction in activity levels.
Sometimes because of the changes the cancer causes in the bone architecture, which is known as osteolysis (eating away), it can weaken the bone, which can eventually fracture. This is a pathological fracture.


Axial
OSA in the mouth may present as bad breath, seeing blood in the food or water bowl or a visible mass near the teeth or gums. If your dog has OSA of the skull bones, the tumour may cause changes in their facial appearance and symmetry, or grow into the brain cavity possibly causing neurological signs such as seizures. Spinal OSA may compress the spinal cord or nerves and may cause your dog to have difficulty in walking, partially or even completely. Rib OSA can manifest as a fixed firm swelling beneath the skin over the rib cage, often about two-thirds of the way down the length of the rib.
What is the cause of OSA?
There is no definitive cause for OSA but it is thought to be related to the genes that both promote and suppress tumour cell growth. It is definitely seen in some breeds more than others, for example, Greyhounds, Great Danes, Mastiffs, Irish Wolfhounds, Dobermanns and Rottweilers. Recent clinical research has also found a correlation between early castration and spaying and appendicular osteosarcoma development in Rottweilers.
How is OSA diagnosed?
Diagnosis aims to not only investigate the primary tumour but also determine the extent of spread of the cancer within the body at the time of presentation. This is known as ‘staging’. It is important to emphasise that not all spread (metastases) may be visible even if all of the body is scanned and that it is common for OSA to have spread at a cellular level by the time of diagnosis of the primary tumour.
Blood work and urinalysis
Taking blood and urine samples are routine procedures. It provides us with invaluable information regarding the general health of the patient, which in turn enables us to develop individual anaesthetic protocols as necessary. It may also provide us with information about the cancer itself, though cancer cells of OSA are not yet possible to pick up on a blood test; they may be someday.
Radiographs
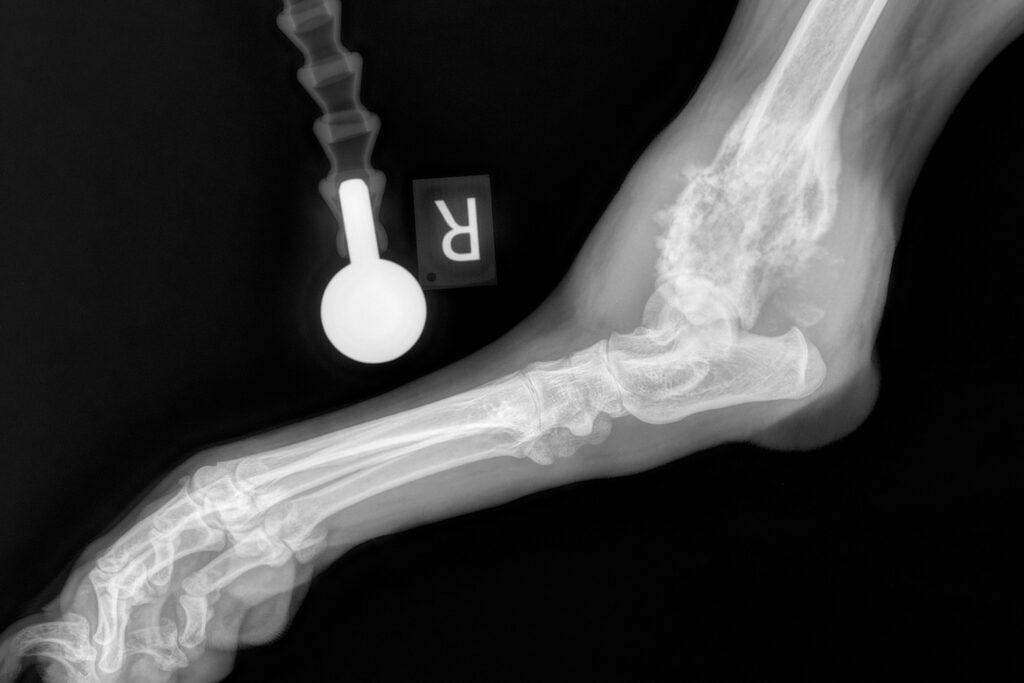
X-ray pictures are taken of the affected limb to rule out any other problems, for example, fracture or infection, and to ascertain the extent of the infiltration of the cancer within the bone and outside the bone in surrounding tissues and neighbouring joints.
Secondly, x-ray pictures can be used to determine the extent of tumour spread to other parts of the body, specifically the lungs, which is the most common site of spread of OSA. It should be emphasised however, that x-ray pictures are not as sensitive for detecting such spread as is a CT scan with a powerful scanner.
Computed Tomography (CT)
A CT scanner uses a narrow beam of x-rays from a generator rotating quickly around a large doughnut-shaped ‘gantry’ through which the patient passes on a table. The x-ray beam passing through tissues of varying density produce signals that are processed by a computer to generate cross-sectional images, or “slices. This is so-called ‘cross-sectional’ imaging and is a much more advanced imaging technique than x-ray pictures. CT scans, especially those from a high-powered machine are able to detect much more subtle changes in a bone affected by OSA and in lung or other tissues to which the cancer can metastasise. CT scans can also be used to reconstruct the bone tumour in 3D to help us to make decisions about whether or not it is possible to save the leg, which is known as limb-sparing surgery.
Bone biopsy
Under sedation, a fine needle can be pushed through a thin defect in the bone wall to collect some cells which can be examined under the microscope to confirm the diagnosis of cancer and elucidate the type of cancer. Sometimes insufficient material is obtained this way, or there isn’t a thin defect in the bone cortex. Then, under general anaesthesia, a thin core of bone tissue can be taken from the area using a special trephine punch and examined under a microscope to confirm malignancy and the type thereof. It is not always necessary to biopsy bone lesions ahead of treatment but your clinician will discuss this process with you. Sometimes biopsy is contraindicated, i.e. not advisable, if one is considering replacing the tumour with a metal implant in limb salvage, because in so doing one may contaminate the surrounding tissue with tumour cells, which is known as ‘seeding’.
How is OSA treated? Appendicular OSA
There is no ‘best’ way to treat bone cancer. Every path we choose depends on discussions with you and your family, i.e. the people who know the patient best. Somewhere below will be an option that is right for you, or it may be a combination of several different options. We will be working with you every step of the way.
Again, it is important to realise that by the time we diagnose OSA, cancer cells have almost certainly already left the primary mass in the bloodstream and have moved to somewhere else in the body, which is known as metastasising. These cells, in clusters or individually, may be too small to detect before surgery, even with the highest-definition CT scans. They can remain dormant for many months before growing into visible tumours. We use chemotherapy to try to slow the progression of these metastatic cells into detectable secondary tumours.
In addition to targeting the cells that have spread, the following options tackle the primary bone tumour, and more specifically, the associated bone pain:
Home care medical management
There are several combinations of drugs we can prescribe which can be given at home. These can be painkillers and anti-cancer drugs used in tandem and can work in different ways to target pain, inflammation and sometimes cancer cell proliferation.
Bisphosphonates
These are bone-hardening drugs originally used in human medicine to strengthen weaker menopausal bone, but their use has evolved to treat bone pain associated with cancer. This drug is given intravenously, typically every 3-5 weeks and can be used in conjunction with a home care protocol. Their use, often very successfully reduces bone pain and can also decrease bone destruction, thus decreasing the risk of pathologic fracture.
In some instances, the tumour may not be removed at all, but rather managed medically with bisphosphonates and pain-killing analgesics for the primary tumour, in combination with chemotherapy for metastases. The idea behind this approach is to utilise the presence of the primary tumour and its tumour microenvironment to stimulate the body’s immune system, which in some cases may delay the development of metastases. Research is ongoing into this approach and the most effective combination of drug therapy, but satisfactory quality of life can be provided for some patients, with sometimes survival duration similar to full limb amputation or limb salvage. Some OSAs can be supported by a plate and screws to bridge the weak bone in-situ if they have fractured or are about to fracture, ‘buying time’ for the limb and providing quality of life for a period of time. We treat every single case on an individual basis with patient-specific protocols of personalised medicine/surgery.
Radiation therapy
Palliative radiation therapy, delivered by a machine known as a linear accelerator, can be used to treat cancer-related bone pain and inflammation in an endeavour to improve quality of life. Depending on the protocol 1-4 doses (‘fractions’) may be administered in a highly-focussed zone, which is known as stereotactic body radiation therapy (SBRT), in conjunction with medical management including bisphosphonates. Radiation only targets the tumour in the bone and does not address any distant metastatic spread. The specific role that radiation therapy may play will be discussed by our clinicians. SRBT may be contraindicated in certain situations such as where pathological fracture has occurred or is imminent. Reports indicate that about half of all cases receiving SBRT progress to fracture and that full limb amputation may result in longer overall survival time versus SBRT. Side effects can include skin breakdown in about one-third of patients.
Amputation
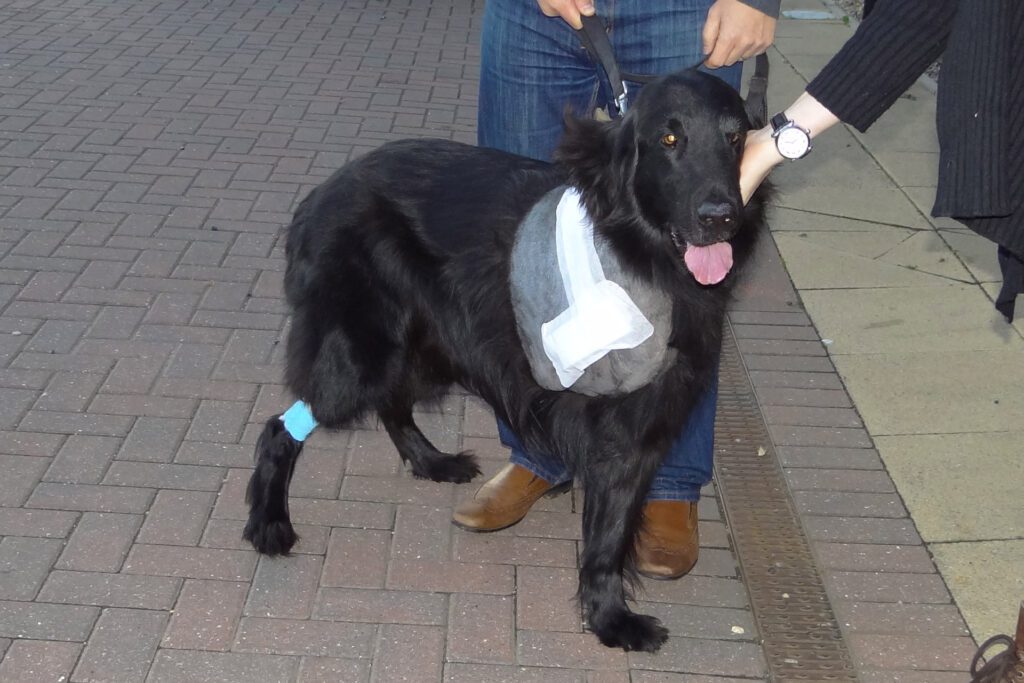
Full limb amputation is well tolerated by most dogs and can provide an excellent quality of life. Amputation of the hind limb is generally better tolerated since the front limbs bear more body weight. Dogs of lower body weight manage better with any full limb amputation, whereas overweight dogs tend to struggle more. However, even giant breed dogs with full amputation of one of the front limbs can manage satisfactorily well with appropriate management and harness support if needed. When making the decision to sacrifice any limb, other factors such as concurrent orthopaedic and neurologic disease need to be considered. For example, osteoarthritis or a nerve problem affecting one of the remaining three limbs needs to be seriously considered.
Sacrificing the affected limb is a common surgical procedure performed to remove the primary tumour, and is the fastest, most reliable and most predictable way to end bone pain, to minimise complications of the bone tumour, and to prevent the development of a pathological fracture.
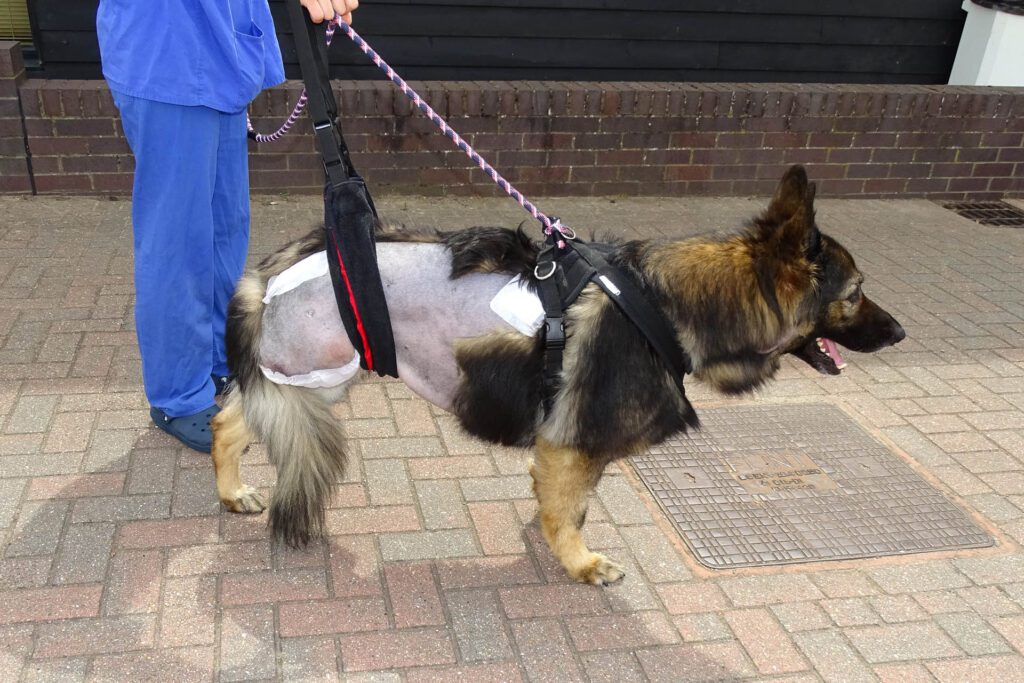



Limb sparing surgery
Limb sparing surgery describes any technique whereby the primary bone tumour is removed without removing the entire limb. Simple examples include removing part of the ulna (ulnectomy), or part of the scapula (scapulectomy) if the tumour is confined to parts of these bones.
If the tumour is in the major long bones that bear most of the dog’s weight; for example, the radius, humerus, femur or tibia, then implants may be used to replace the bone removed when resecting the tumour. An internal prosthesis is called an endoprosthesis. It is effectively a shaped piece of metal which fills the bone defect where the cancer bone was, and is attached to the adjacent bone(s) with plates and screws, often involving fusion of a joint. The most common endoprostheses are employed to replace tumours of the bottom part of the forearm (radius and ulna) or shin bone (tibia), and in both scenarios the joints below are fused – the wrist (carpus) or the hock (tibio-tarsus). But endoprostheses can also be used to replace femoral tumours, with a customised hip replacement if the tumour is at the top of the bone, or a customised knee replacement if the tumour is at the bottom of the bone. Endoprostheses can also be used to replace tumours of the humerus bone with fusion of the shoulder (scapula-humeral endoprosthesis). Professor Noel Fitzpatrick has developed implant systems for all of these limb salvage scenarios over the past two decades, which are manufactured to his specification and are uniquely offered by Fitzpatrick Referrals.
Professor Noel Fitzpatrick has also developed another innovative amputation endoprosthesis which is called a PerFiTS implant (Percutaneous Fixation To Skeleton), which is also only available at Fitzpatrick Referrals. This is used to treat animals where the lower part of a limb is obliterated beyond salvage either by cancer (bone or soft tissue), or by severe trauma to bones, muscles, nerves and/or blood vessels. This particular endoprosthesis has three components. The first attaches to the bone inside the limb using a rod, plates and screws. The second is a special mesh called the dermal integration module, onto which the skin can adhere with the aim of forming a permanent seal. And the third is a solid metal rod called a spigot onto which an external ‘foot’ can be attached, which is known as the exoprosthesis.
These techniques are highly specialised surgical procedures which are carefully tailored to the individual dog and family, taking account of the practical, financial and ethical implications for every individual case. Due to the unique decades-long collaboration between Professor Noel Fitzpatrick and his engineering colleagues, no centre in the United Kingdom has more experience in surgical limb sparing techniques than Fitzpatrick Referrals.
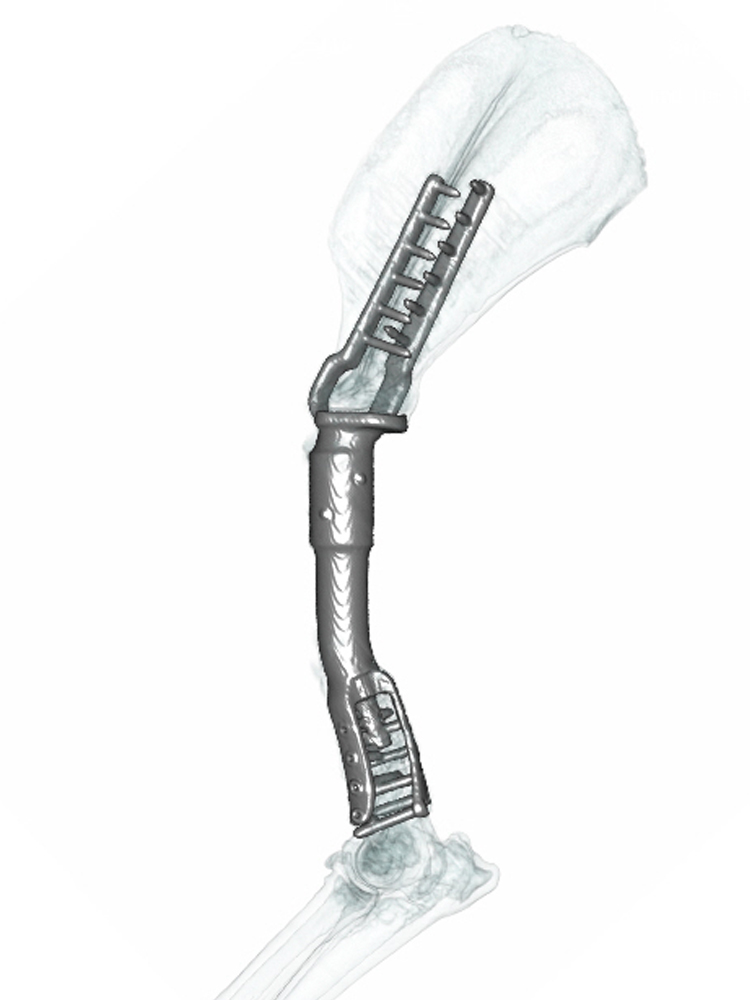
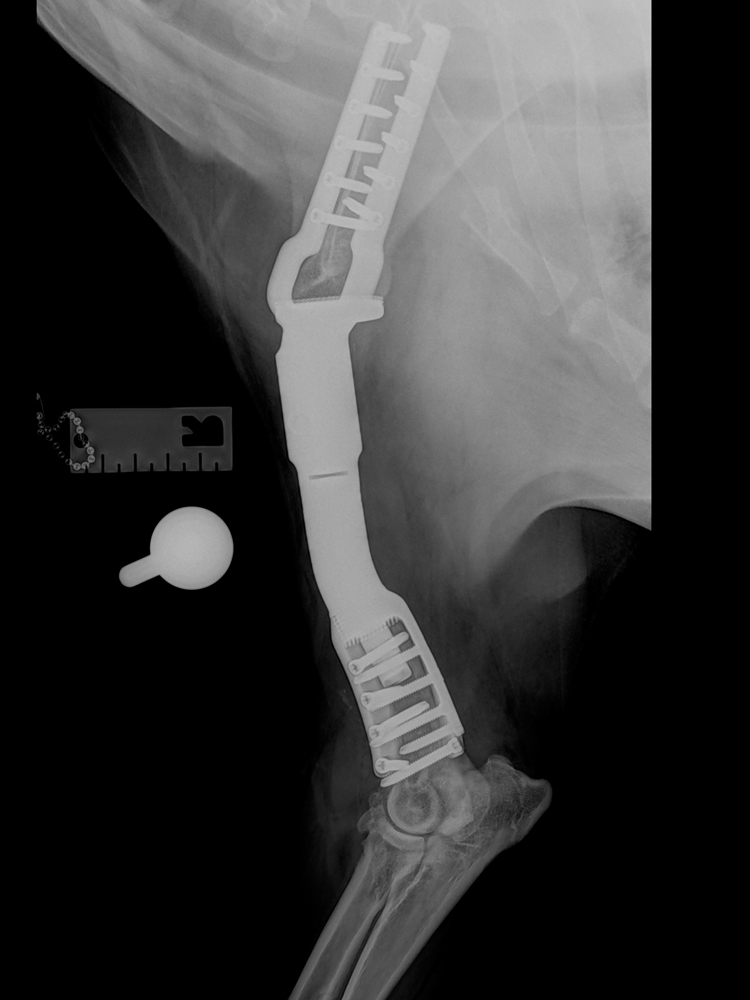
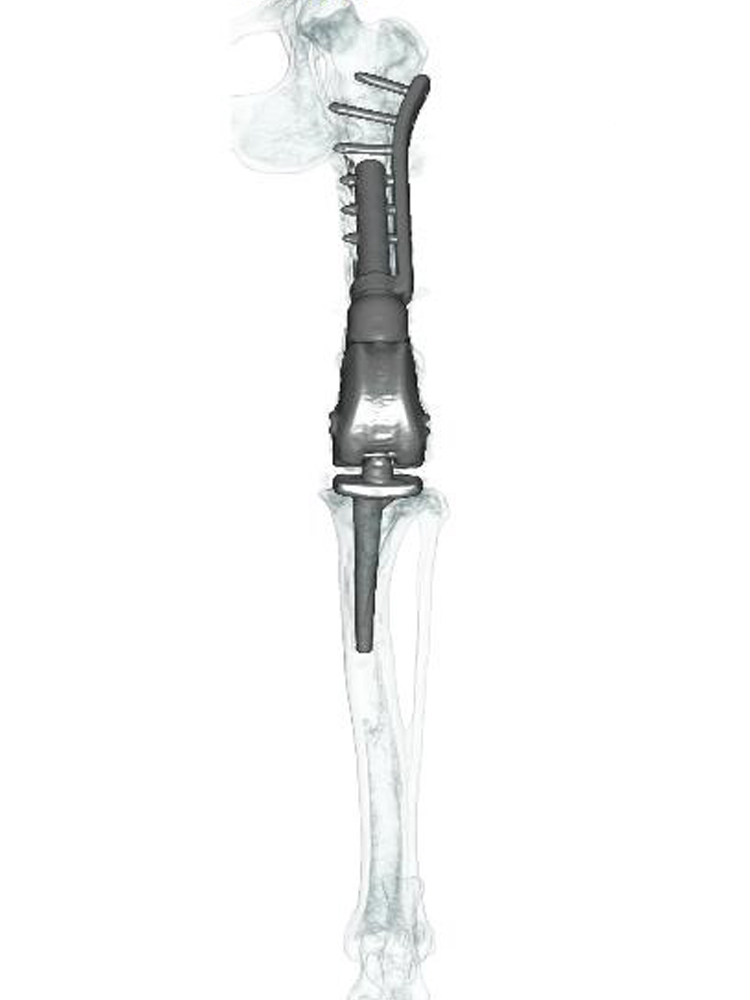
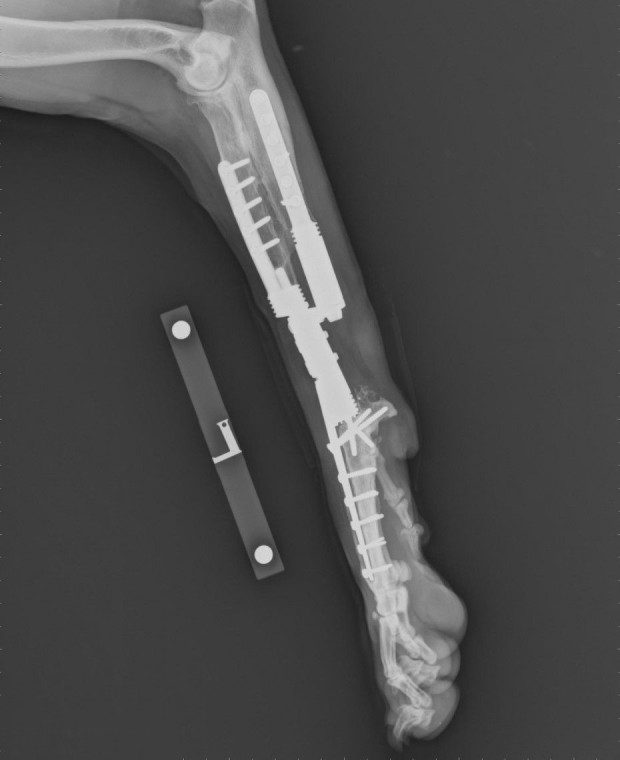
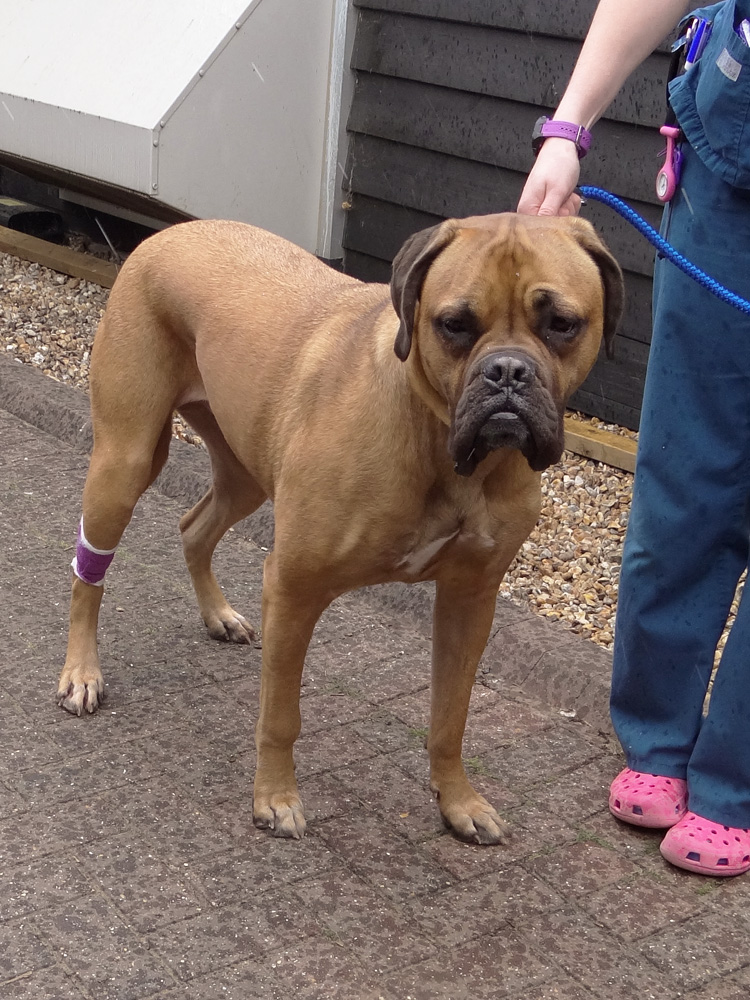
Patients with PerFiTS


Chemotherapy
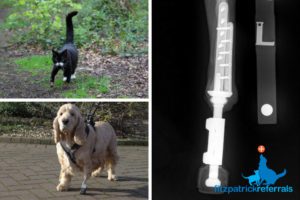
The number one goal of treating OSA is the relief of bone pain and the re-establishment of a good quality of life. The second goal is longevity – we know for a fact that chemotherapy extends the life of dogs suffering from long bone OSA. The treatment regime we employ is typically an intravenous injection of chemotherapy drug every three weeks, most often a drug called carboplatin. Intravenous access can be gained by placing an IV cannula every three weeks or so for four or five times administration, which doesn’t trouble most dogs, or by using a plastic tube placed in a vein which is attached to a vascular access port (VAP).
Here at Fitzpatrick Referrals, our team of dedicated clinicians and nurses have many years of experience in delivering chemotherapy treatments for OSA, We adhere to the strictest safety standards for reconstituting, delivering, and disposing of chemotherapy drugs and waste. Our goal is to make our patients as comfortable as possible with the least upset and to educate families regarding all aspects of the disease.
Dogs do not normally experience the same side effects as people, although we do occasionally see transient inappetence, nausea, lethargy and loose stools. We use drugs to try to prevent side effects, and if side effects do occur, they usually don’t last beyond a day or two. Most of your friends and family would have no idea that your canine friend is receiving chemotherapy.
How is OSA treated? Axial OSA
The treatment for axial OSA usually depends on the location of the tumour. Some of the same options exist as above for axial OSA, such as medical management including bisphosphonates, radiation therapy, surgical removal and chemotherapy.
Surgery for axial OSA might, for example, involve removing an affected rib, or part of the jaw or the pelvis, all with appropriate reconstruction techniques. Dogs can often manage very well without part of their jaw or pelvis, and at Fitzpatrick Referrals we have pioneered customised jaw (mandibular) and pelvis implants, including replacement of joints if this is deemed most appropriate in a specific patient.
What is the prognosis of OSA?
Despite all our best efforts, dogs with appendicular (long bone) OSA will almost certainly be lost to the disease, either from the primary tumour (the bone) causing uncontrollable pain, or the secondary tumours (the metastases) affecting the quality of life to the extent that euthanasia is indicated. The commonest site of metastatic spread is to the lungs, and advanced disease in the lungs most commonly causes weight loss and weakness (cachexia), rather than breathing problems which you might expect.
The following factors can influence prognosis; presence of tumour spread to the lungs at diagnosis, how aggressive the tumour is determined to be by histopathological analysis, specific elevations in blood parameters, spread of disease to regional lymph nodes, whether or not chemotherapy is given, which bone is affected, the weight of the patient, and the age of the patient.
Two things are important to realise. The first is that most tumours present to referral centres quite late in the disease process. The second is that since survival time is measured from the time of diagnosis, the earlier the diagnosis and referral for treatment is made, generally the better the outcome. So, once a dog presents as lame and pain is identified associated with a long bone or a swelling of the bone is noticed, prompt action is warranted.
Median survival times have been reported for the following therapies. It is important to realise that these numbers are averages – half the patients will do better than these figures, but half, unfortunately, will do worse.
- Amputation and chemotherapy – 10 to 12 months
- Limb spare and chemotherapy – 10 to 12 months
- Radiation and chemotherapy – 8 to 10 months
- Amputation alone – 4 to 5 months
- Palliative care only (painkillers without chemotherapy) – varies, but can be approximately 1 to 3 months
21 minute read
In this article