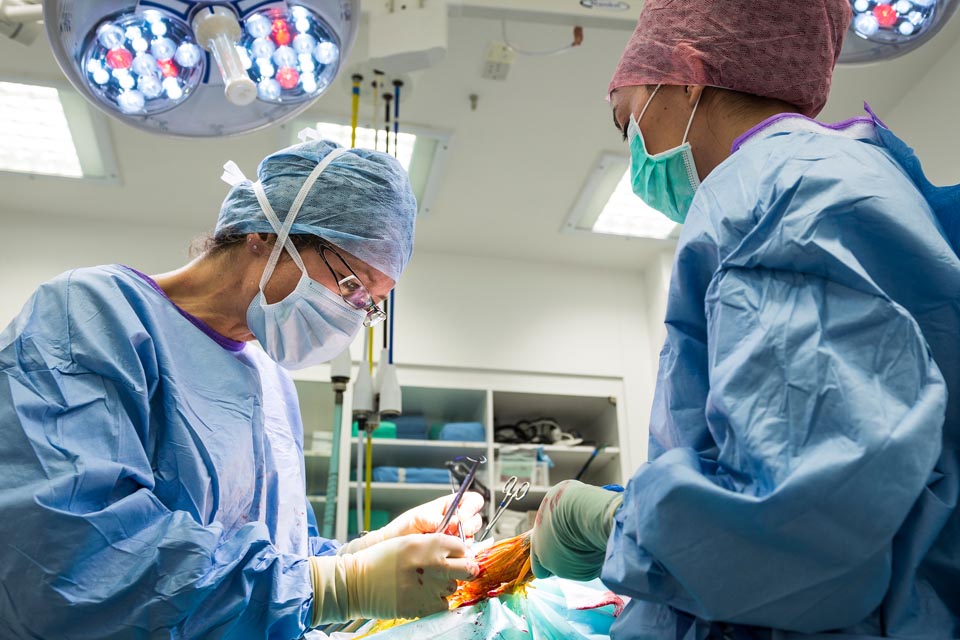
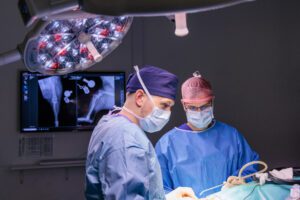
By Dr Sarah Girling
Senior Surgeon, OrthopaedicsHealthy, active, pain-free pets are important family members. But our pets do not speak and we should be able to understand when they are in pain.
Unfortunately, hip dysplasia (HD) is an all too common, developmental orthopaedic condition resulting in osteoarthritis (OA). Osteoarthritis causes discomfort, chronic aching and pain. So it is important for the primary care vet to engage with the insidious nature of this condition and recognise the varying manifestations of pain and furthermore when to act and refer to a specialist.
Recognise and differentiate the varying degrees of pain
Acute pain may manifest as restlessness or difficulty getting comfortable, struggling to get up, or a sudden reaction to unexpected pain which manifests as whining, crying, biting or hiding or escaping. Chronic pain gives the appearance of tolerance, often without perceived signs of pain or lameness. Equally the patient’s family perceives pain and describes this to manifest as an altered gait or altered behaviour. Recording a patient’s daily level of activity provides a very objective measure for review, and a useful indicator when assessing response to treatment.
We predominantly see our patients at two phases as hip laxity progresses to coxofemoral osteoarthritis. Typically, phase one is the juvenile patient (five to twelve months) suffering from hip laxity, whereby the femoral ligament is stretched and oedematous, joint fluid is increased and the joint capsule is stretched at the origin and insertion points. Phase two is the mature patient with developed osteoarthritis; the original strain on the joint capsule, inflammation and increased joint fluid progresses to joint capsule thickening and periarticular fibrosis.
When do I refer?
Identifying the stage the patient is at assists the veterinarian’s understanding of underlying pain and combined with an assessment of the impact on the patients’ quality of life, will allow you to develop an appropriate course of treatment. If you ever need assistance with radiographs and imaging or would prefer to seek surgical treatment from a specialist, don’t hesitate to get in touch.
Management options
Management is divided into medical/conservative (exercise modification, pharmacologic/analgesia and rehabilitation) and surgical. Radiographic assessment with examination of joint laxity (Bardens or Ortolani sign) under anaesthesia enhances the veterinarian’s understanding of the individual’s condition. Furthermore, if osteoarthritis is not evident, then the patient may be appropriate for early surgical intervention such a pubic symphysiodesis (JPS) or double pelvic osteotomy (DPO).
| Phase one juvenile: treatment options | Phase two mature: treatment options | |
| Medical management | Multimodal analgesia | Multimodal analgesia |
| Neutraceuticals | ||
| Rehabilitation | Exercise modification (restricted activity should only be temporary) | Exercise modification |
| Physiotherapy and hydrotherapy | Physiotherapy and hydrotherapy | |
| Surgical | Juvenile Pubic Symphysiodesis (JPS) | Total Hip Replacement (THR) |
| Triple or Double Pelvic Osteotomy (TPO/DPO) | Femoral Head and Neck Excision (FHNE) | |
| Total Hip Replacement (THR) | ||
| Femoral Head and Neck Excision (FHNE) |
Total hip replacement and the mature patient
Total hip replacement (THR) is a long term solution to hip pain for the immature and mature patient. Osteoarthritis will never go away and the impact on the patient is insidious.
The success rate is 95% and the patient regains normal gait, trot and gallop, normal activity, and they are free of chronic aches and pain.
At Fitzpatrick Referrals, we use the universal BioMedtrix THR system which comprises CFX (cemented) implants made from cobalt chromium alloys and BFX (biological) implants made from titanium alloys with a cobalt chromium articulating head. The CFX Micro and Nano hip system is our primary recommendation for small breed dogs and cats affected by SCFE (slipped capital femoral epiphysis), osteoarthritis, avascular necrosis or femoral head fracture failure. It provides a superior functional and pain-free improvement when compared to FHNE.
What to expect?
At initial consultation, we take the time to help the families appreciate the importance of hip pain and osteoarthritis as a lifelong condition. We provide information and manage expectations to help with family decision-making and to ensure they are comfortable with post-operative care, complications and the appropriate timing of any surgical intervention. At the same time, radiographic assessment is performed.
A second appointment is then made for surgical intervention. It is important that patients do not suffer any obvious infection (dental disease, pyoderma, pyometra, UTI, otitis externa) in the weeks immediately prior to surgery, as this would increase the risk of post-operative infection. Patients remain with us for three to five days and are discharged when we are satisfied their pain is adequately managed.
Post-operative confinement and exercise control is essential to reduce the key complications of prosthetic dislocation. Clients who do not wish to comply with this regime should be discouraged from embarking on this journey.
At discharge, we provide physiotherapy guidelines and help the patient into the car. Further re-examination is planned for six and twelve weeks post-surgery. Physiotherapy follow-up is provided as necessary.
Tailored treatment plan
Remember we tailor a treatment plan for the individual; no two patients with this condition are the same and all respond differently.
Patient advice for vets
If you need help to interpret radiographs or to decide on a treatment plan, please phone 01483 423761 or email [email protected] to discuss or send your patient along for an assessment.
Read more about our orthopaedic service and rehabilitation service
Read our client pages on hip dysplasia and total hip replacement surgery
4 minute read
In this article