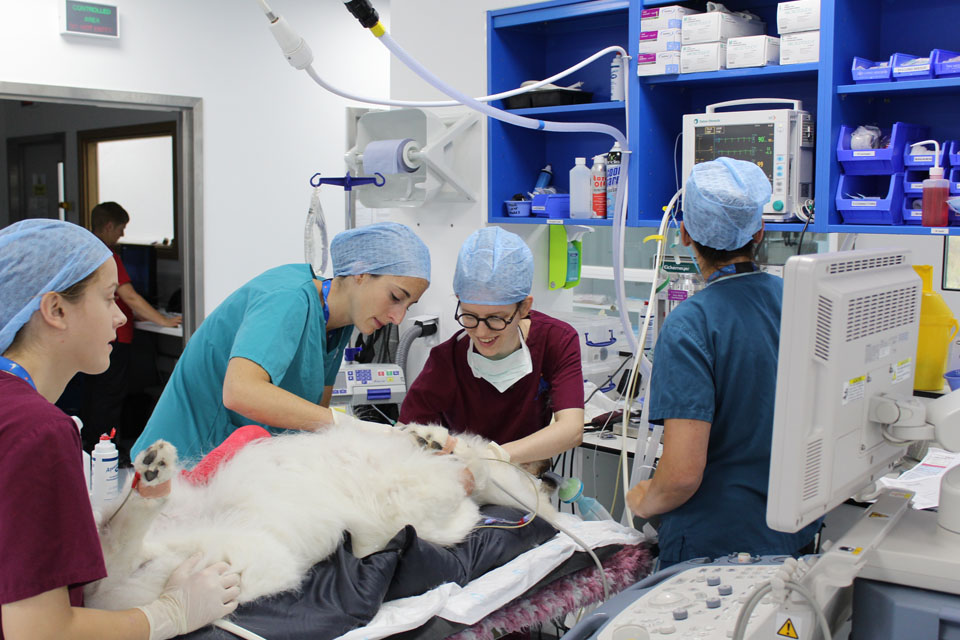
We understand it’s a worrying time when your pet has to go in for a diagnostic work-up and/or surgery and that anaesthesia can be another worry for clients on top of the procedure itself.
Fitzpatrick Referrals’ Anaesthetist Daisy Norgate guides you through the process and answers some of the frequently asked questions we receive about anaesthesia to mark World Anaesthesia Day. <!– wp:uagb/image {“block_id”:”m4qteKNm”,”url”:”https://www.fitzpatrickreferrals.co.uk/wp-content/uploads/2019/10/IMG_4129-Patient-having-ultrasound-960×640.jpg”,”enableCaption”:true,”caption”:” Anaesthetist Daisy Norgate performing an ultrasound-guided local block prior to the patient having surgery.”,”align”:”center”,”id”:1683,”linkDestination”:”none”,”width”:960,”height”:847,”naturalWidth”:925,”naturalHeight”:900,”sizeSlug”:”full”,”sizeSlugTablet”:”full”,”sizeSlugMobile”:”full”} –>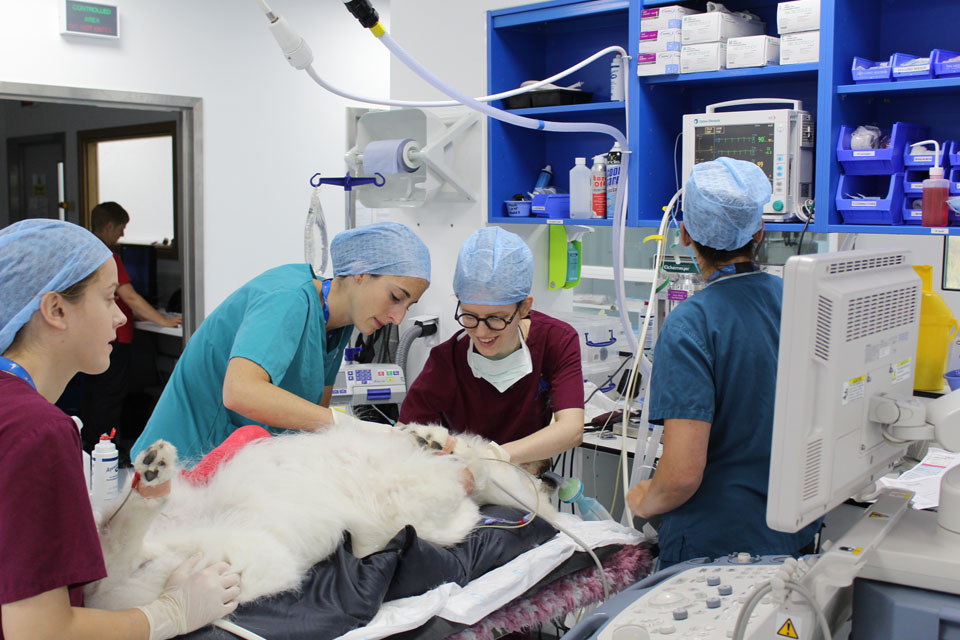
What is anaesthesia?
Anaesthesia means loss of consciousness and sensation. A lot of procedures and most operations can only be performed whilst an animal is under anaesthesia. Anaesthesia comprises of three main components which are produced by using a combination of anaesthetic drugs:- Hypnosis – the animal loses the ability of voluntary movement
- Muscle relaxation – the muscle is in its resting state
- Analgesia – relief of pain
What is the role of an anaesthetist?
An anaesthetist is a veterinary surgeon that has undergone at least an additional three years specialist training just in the field of anaesthesia and analgesia. Day to day as an anaesthetist I will oversee a team of nurses who will be one on one with every patient being anaesthetised. Together we will assess every patient and decide on an appropriate anaesthetic plan tailored to each individual. If any adverse events occur under anaesthesia, then I will ensure that these are corrected as soon as possible to prevent any long-lasting issues. Other clinicians will also seek my advice on pain assessment and management in both awake patients and those under anaesthesia.
What information does the anaesthetist need to know about the patient before a general anaesthetic (GA)?
The most important information to acquire before an anaesthetic is the most recent clinical history which will reveal ongoing medical conditions and ongoing medications. This information may alter the drugs used during the anaesthetic and will also allow highlight if the patient is at a greater risk of certain adverse events under anaesthesia which then can be prepared for prior to the actual induction of anaesthesia.What checks do you do before a patient is put under GA?
All patients will have a full physical exam with specific attention paid to heart and lung auscultation, hydration status and overall demeanour. This will flag up any undetected heart murmurs or subclinical disease. Identifying the temperament of the patient is also very important. Pre-operative bloods are routinely checked in geriatric patients or those that might give some suspicion of potential subclinical disease.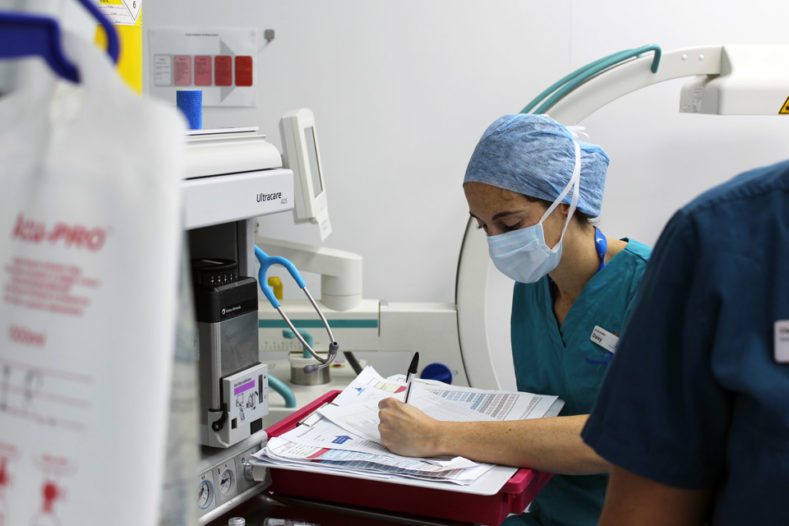
How do you keep animals warm when under anaesthesia?
Warming of patients is implemented in every single patient undergoing anaesthesia unless they have a very high temperature beforehand. This is because rapid heat loss and hypothermia is very common in anaesthetised patients, which can then prolong recovery. Patients are actively warmed using specific devices that either provide heat through a matt that lies underneath the patient or via a blanket or a container filled with hot ait that surrounds the patient. Active warming is implemented in the immediate period prior to induction of anaesthesia and is continued into the recovery period until the patient’s temperature returns to normal.What are the risks involved with anaesthesia?
Overall, the risks involved with anaesthesia in a healthy patient are very low. However, certain risks may increase depending on the species, breed or health status prior to the induction of anaesthesia. Each patient undergoing an anaesthetic is given a physical status classification ranging from 1 (a normal healthy patient) to 5 (a severely ill patient who may not survive without the surgery) and as the number increases the probability of adverse events under anaesthesia also increases. Specific breeds are also associated with an increased anaesthetic risk and the main ones documented are any brachycephalic (relatively broad and short skull) breeds such as the Pug or French Bulldogs. These patients have increased airway risks due to their skull conformation.Why is it important for patients to be starved before anaesthesia?
Patients are starved for anaesthesia so that they do not have a full stomach and therefore have a reduced risk of vomiting. This is particularly important in anaesthetised patients as they are unable to maintain their gag reflex and therefore protect their airway from any potential vomit or regurgitation. Patients should also not be starved for too long periods of time as this will also increase the risk of vomiting and regurgitating.For elderly dogs or cats, are there more risks involved with GA? Can an animal be too old or too young to be anaesthetised?
A geriatric animal is one that has reached 80% of its life expectancy so the age at which an animal is deemed geriatric is dependent on its species and breed. At this point, the body’s organs don’t function as well and therefore drug metabolism is a bit slower so animals need less drugs and recovery may be longer. Despite knowing this, if a patient requires an anaesthetic for diagnostic purposes or a surgery that will improve its quality of life then it can be justified to go ahead with the anaesthetic despite the increased risk. Overall, you can’t really dictate whether an animal is either too old or young for an anaesthetic, it’s about weighing up the risks and benefits of the anaesthetic and outcome and ultimately making the decision to proceed based on what is morally and ethically best for the patient. <!– wp:uagb/image {“block_id”:”kDa4eTmp”,”url”:”https://www.fitzpatrickreferrals.co.uk/wp-content/uploads/2019/10/IMG_4210-Anaesthetist-Daisy-monitoring-patient-during-surgery-960×640-789×526.jpg”,”enableCaption”:true,”caption”:” Anaesthetist Daisy Norgate monitoring a patient during surgery.”,”align”:”center”,”id”:1686,”linkDestination”:”none”,”width”:789,”height”:847,”naturalWidth”:925,”naturalHeight”:900,”sizeSlug”:”full”,”sizeSlugTablet”:”full”,”sizeSlugMobile”:”full”} –>
Is it safer for dogs to be sedated versus general anaesthesia?
The decision to either sedate or fully anaesthetise a patient primarily depends on what procedure needs to be performed. In general, sedation is used when just imaging needs to be done and general anaesthesia is performed for all surgeries. Both sedation and general anaesthesia are very safe in your average healthy patient so the risk will vary with each technique depending on your patient. For example, general anaesthesia may be safer than sedation in brachycephalic dogs as then they will definitely have their airway protected. On the other hand, general anaesthesia tends to be longer than sedation and therefore there is more time for unwanted events to occur. Overall, the answer to this question depends on the individual patient.How long does it take for a patient to recover after anaesthesia?
The length of recovery of a patient after anaesthesia depends on many factors such as the drugs used perioperatively, the procedure performed, the physical status of the animal beforehand and the degree of anaesthesia. Generally, the immediate recovery period can range from 15 minutes to 2 hours. Efforts are made to make this period as short as possible.How has anaesthesia changed over the years?
Over the last 10 years, veterinary anaesthesia has changed drastically. Practice standards have been introduced dictating that each patient undergoing anaesthesia must be attached to the minimum basic monitoring so that early warning signs of potential complications are picked up and addressed before a major event occurs. Accessibility to monitoring devices has also increased resulting in more and more veterinary surgeons using them routinely. The knowledge and practice of local regional anaesthesia in veterinary species has also increased hugely resulting in targeted analgesia of specific sites and therefore the decreased necessity of systemic analgesic drugs leading to less unwanted systemic side effects. Technology is also increasing rapidly which has many potential benefits for the future of veterinary anaesthesia.
SHARE
7 minute read
In this article
We understand it’s a worrying time when your pet has to go in for a diagnostic work-up and/or surgery and that anaesthesia can be another worry for clients on top of the procedure itself.What is anaesthesia?What is the role of an anaesthetist?What information does the anaesthetist need to know about the patient before a general anaesthetic (GA)?What checks do you do before a patient is put under GA?How do you keep animals warm when under anaesthesia?What are the risks involved with anaesthesia?Why is it important for patients to be starved before anaesthesia?For elderly dogs or cats, are there more risks involved with GA? Can an animal be too old or too young to be anaesthetised?Is it safer for dogs to be sedated versus general anaesthesia?How long does it take for a patient to recover after anaesthesia?How has anaesthesia changed over the years?
SHARE