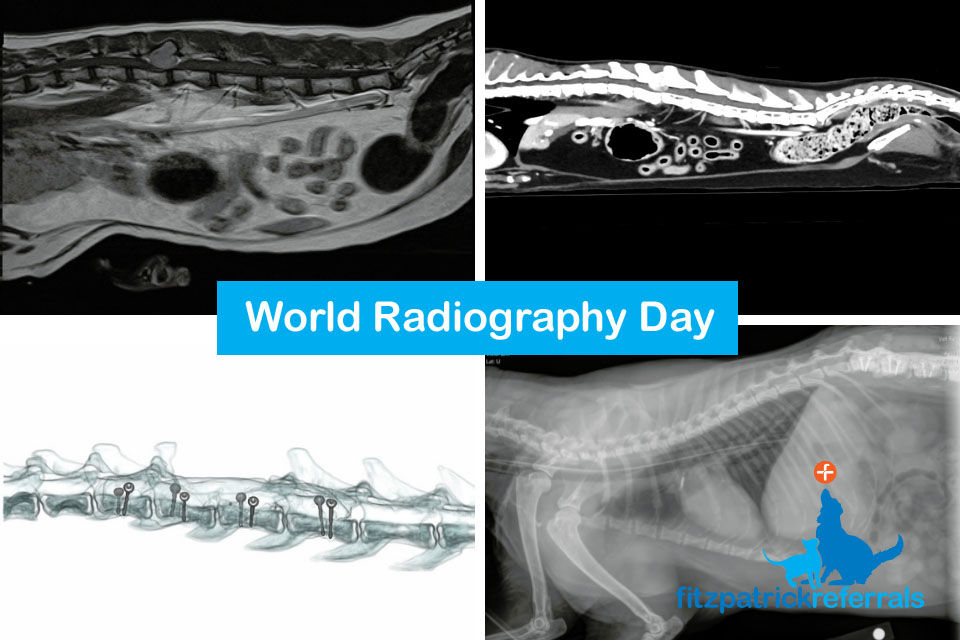
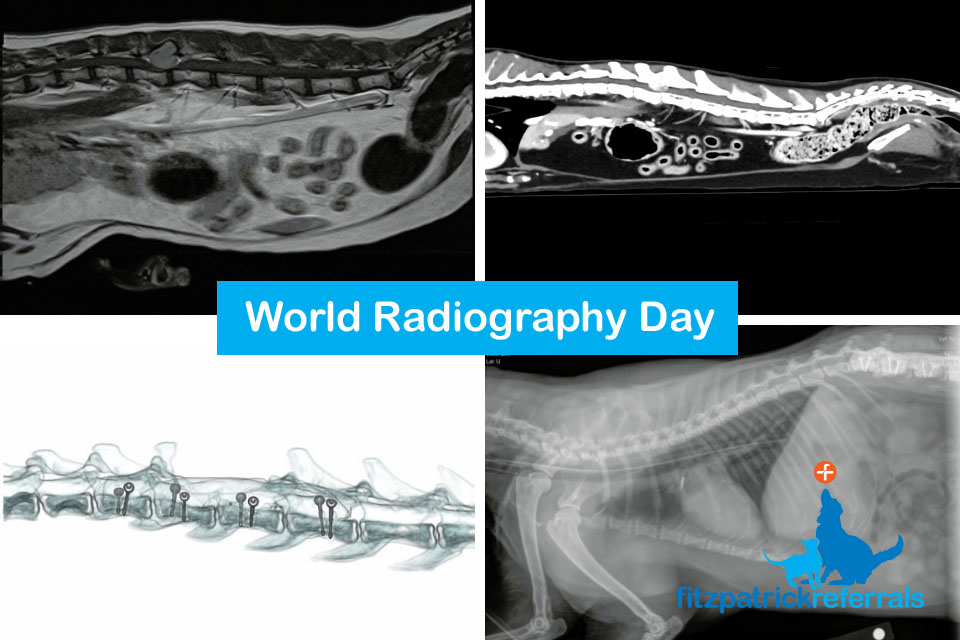
For World Radiography Day, we caught up with our radiography team to explore three of the imaging options that we use regularly and their pros and cons, which help our specialists diagnose and plan surgeries and/or treatments for patients in our care.
We also look at the case example of ‘Doug the cat’ to show how the different modalities were used from diagnosis to pre and post op imaging and aftercare and to explain why it was used. The 10-year-old male feline patient had MRI, CT and x-ray imaging during his stay at Fitzpatrick Referrals, under the care of Professor Clare Rusbridge from our neurology team. We’ll be sharing his full patient story in the coming weeks.
MRI – Magnetic Resonance Imaging
MRI uses a powerful magnet, radio waves and a very sophisticated computer. The advanced technology relies on water molecules, or in particular hydrogen protons, which are abundant in every part of the body. When in a strong magnetic field the protons all align – they are then knocked out of alignment by a radio wave. When the radio wave is turned off the protons begin to realign sending out a signal. Protons in different structures will realign at different speeds and send out different signals and from this, the computer can work out which structures are where. MRI scans are run in lots of little sections or ‘sequences’ with each sequence designed to demonstrate the anatomy and pathology in different contrasts.
Pros
- Excellent differentiation between soft tissue structures, modality of choice for the central nervous system
- No ionizing radiation involved
- No iodinated contrast used (Gadolinium contrast has a lower risk of adverse reactions compared to iodinated contrast used in CT)
- Variety of sequences available that can be tailored to specific patient conditions
- Can assess vascularity with and without use if contrast
Cons
- Long scan times
- Implant safety needs to be considered – any implant going into the high magnetic field needs to be signed off as MRI safe, so it’s important to know the type of implant used in previous surgical procedures and when this surgery was carried out.
- Expensive
- Not as readily available
- Sequences can be noisy
- GA required
Common pathologies
Intervertebral disc disease, soft tissue tumours, epilepsy, syringomyelia, vestibular pathology, stroke, ligament and tendon ruptures
Patient case example – Doug the cat
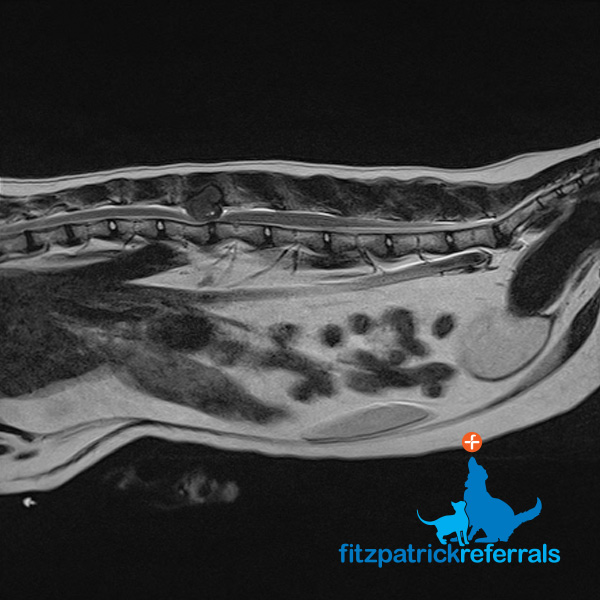
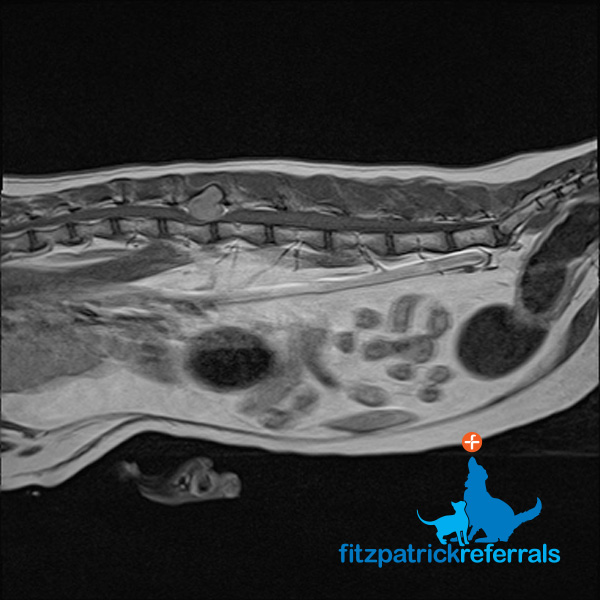
An MRI scan was performed due to the cat’s clinical signs which included dragging his back end, delayed reaction in the pelvic limbs and pain in the lumbar area. These signs pointed to a neurological pathology and after a neurological examination, Chief of Neurology Professor Clare Rusbridge localised the problem to the thoraco-lumbar area. MRI can provide excellent differentiation between soft tissue structures and is, therefore, the best imaging modality to visualise the spinal cord, discs and nerves. MRI showed a tumour at the level of the L2 vertebral body, the tumour looked bony in origin and was severely compressing the spinal cord.
CT – Computed Tomography
A CT scanner also uses x-rays, but instead of having a static x-ray tube and detector, both move 360 degrees around the body continuously emitting x-rays while the table moves through the scanner. This means that three-dimensional data sets are acquired which can then be retrospectively reformatted into any plane of the body using the advanced computer software. As with plain film x-ray, dense structures appear whiter and less dense structures darker.
Pros
- 3D imaging and multiplanar reformatting
- Sensitive to most major organs in the body
- Excellent bone and lung resolution
- Relatively fast scan times
- Can assess vascularity with use of contrast
- Reduces the need for exploratory surgeries
Cons
- Higher radiation dose
- More susceptible to metal artefact
- More expensive than plain film x-rays
- Not as readily available
- Sedation/GA required
Common pathologies
Oncology staging, further assessment of complex fractures and deformities, coronoid disease, surgical planning, lung pathology e.g. pleural effusion, haemothorax, post-operative implant assessment
Patient case example – Doug the cat
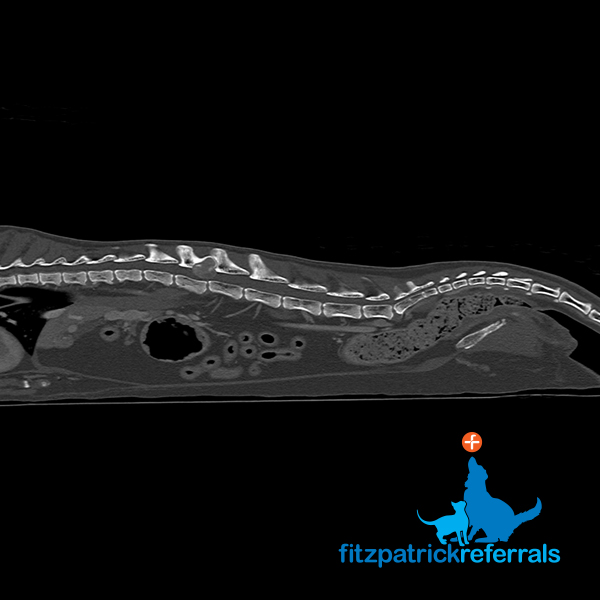
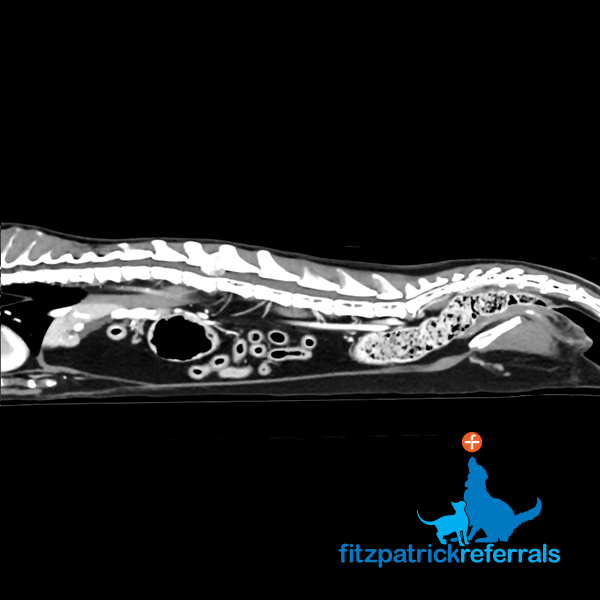
A CT body scan was performed immediately after the MRI in order to stage the tumour and ascertain if there was any cancerous spread. As opposed to an MRI scan which mainly focuses on one body area, CT scans can acquire extensive data from multiple body parts in a short amount of time and are sensitive to most major organs. This makes CT the modality of choice for investigating tumour spread and gaining a good overview of what is happening in the rest of the body. There was no evidence of secondary tumours on the CT and surgical removal of the tumour was offered. The CT also doubled up as a surgical planning tool, as it provides sub millimetric detailed images of the bony anatomy.
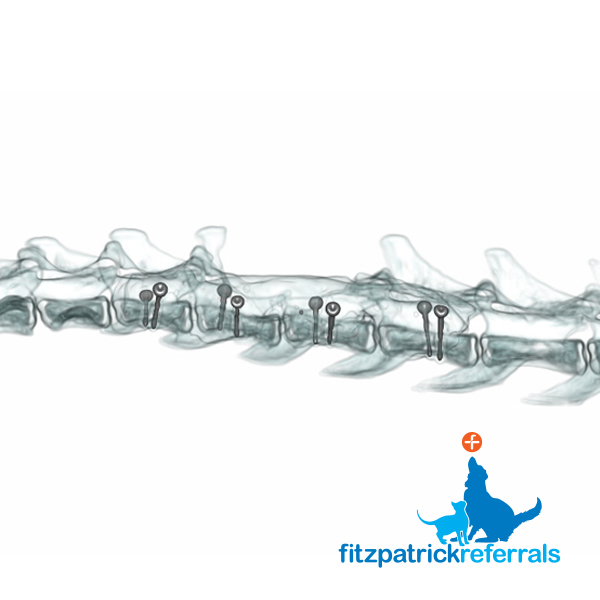
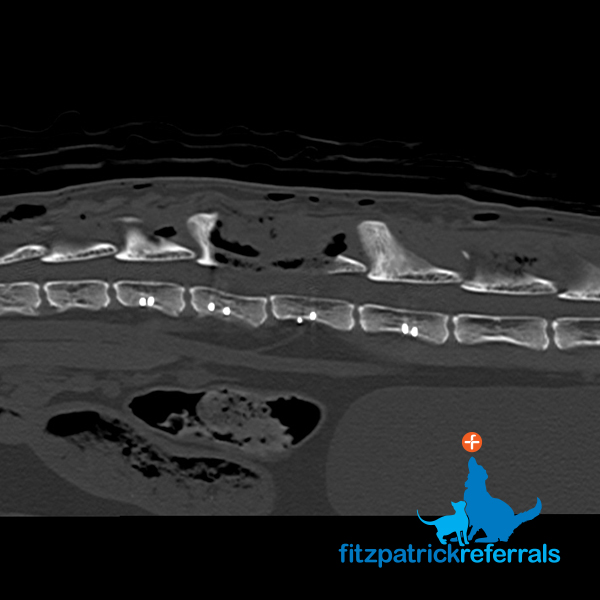
The tumour was resected and part of the affected vertebral body removed. Due to a significant amount of diseased bone being removed the spine was now considered unstable, so pins and cement were placed to act as support for the spinal column. A post op CT was performed in order to check the placement of the pins. CT provides three-dimensional data which can be manipulated into any plane and provides a cross-sectional image of the body which ensured the implants were anchored into the remaining bone of the spine and not the spinal cord.
X-ray
X-rays are emitted from a source (x-ray tube) and projected through the patient onto a detector. As the x-rays pass through the different structures in the body the varying densities will alter how many x-rays reach the plate and the energy of those x-rays. It can then be calculated which structures the x-rays have passed though and where they are in the body. Dense areas (such as bone) are whiter on the images while less dense areas (like air) appear darker.
Pros
- Readily available
- Cheaper
- Quicker
- Low radiation dose
- Provides a good overview in a trauma situation
- Not susceptible to metal artefact
- Can be performed conscious if necessary
Cons
- 2D imaging only, anatomic structures can end up overlying each other on the image
- Provides basic anatomical information
- Good for only a few tissue densities
- Limitations for surgical planning
Common pathologies
Fracture, pneumothorax, arthritis, cruciate ligament disease (though sometimes MRI is needed for further assessment), hip dysplasia, growth deformity, marker films
Patient case example – Doug the cat
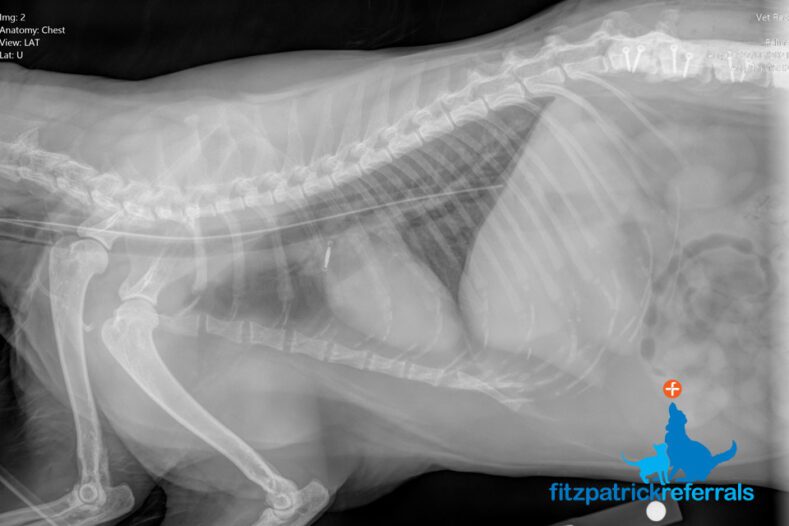
After such a major surgery Doug understandably did not feel much like eating and in order to help him with this, a feeding tube was placed. An x-ray was carried out to check the placement of the feeding tube, which is radiopaque and can therefore be clearly visualised on a 2D thoracic image. X-ray was used as it provides good basic anatomical information in a quick and efficient timeframe and allowed the team to easily confirm the location of the feeding tube.
Read more about our Advanced Diagnostic Imaging (ADI) service
Read Doug’s full patient story
7 minute read
In this article